
News

The classification of seizures and epilepsy has changed greatly over the decades. In 1980 we referred to grand mal seizures, that were convulsions: petit mal seizures that were blank spells; and psychomotor seizures in which individuals go blank and may fiddle with their hands.
In the 1990s we had generalized tonic-clonic, absence, simple and complex partial and secondarily generalised seizures. At present, and we know that this will change again, we have focal aware seizures, focal unaware seizures and focal to bilateral tonic-clonic seizures.
We also now classify seizures by detailed descriptions of what happens at the start of and during the seizures, as this helps us to determine where in the brain a seizure may be starting, which is very important if we are considering the possibility of surgical treatment. We also now understand that seizures do not just involve the grey matter of the brain but also the white matter, which are in effect the wires that join up the different parts of the brain.
Importantly, we recognise now that epilepsy is not a condition in its own right, but is a symptom of a whole range of conditions that affect the brain, and which are often seen alongside other difficulties such as problems with memory or learning, and depression. We recognise that the main causes of epilepsy can be bracketed into groups: genetic disorders, difficulties with brain development and early life, insults to the brain such as infection, tumour, stroke and trauma; and brain degeneration, which is common in older life.
In 1980 there were very few adult or paediatric neurologists. Neurologists would essentially see a patient once, give an opinion, and general practitioners would have to follow through on treatment and following the patient. Hospital care was primarily by general physicians and paediatricians, there were no specialist nurses and, in general, epilepsy was not a priority for primary care.
Nowadays there is continuity of care by neurologists and specialist nurses. Currently there are over 700 epilepsy specialist nurses in the UK. Every regional neurology centre has one or two neurologists, specialising in epilepsy and managing complex cases.
As before, however, general epilepsy is not a priority for general practitioners, who have the whole range of health conditions to deal with.
I predict that in the future, neurologists will focus on diagnosis and the pathways of investigation, with treatment advice driven by algorithms and medication follow-ups will be largely taken on by pharmacists following algorithms.
Call centres will operate with 24/7 access to clinical records, with administrators and nurses giving ongoing care using automated processes.
This may be efficient and effective for some, but a concern will be the loss of the continuity and personal attention that we are trying hard to provide.
In the 1980s this essentially comprised of family members listening out for a person. Currently, wrist-worn sensors detect movements and physiological changes, and implanted ECG recorders monitor heart rate and rhythm.
We are seeing the beginning of implanted EEG recorders for determining epileptic activity.
I think that, in the future, we will see monitoring and treatments working symbiotically.
Implanted EEG detectors will be linked to a system for delivering antiseizure medication directly into the brain, at the time and at the place it is needed.
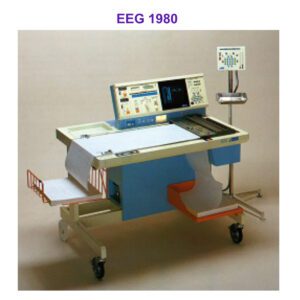
An EEG is a test that records electrical activity in the brain, and it has been the mainstay of helping to diagnose epilepsy.
In the 1980s, these comprised pen and ink recorders with pages and pages of printed records and the interpretation of the traces relied primarily on pattern recognition by a skilled neurophysiologist.
Nowadays, EEGs are digital, with automated assessments to identify any abnormalities indicating seizure propensity and where in the brain they arise.
In the future, I expect that we will have artificial intelligence-based models for detecting electrical abnormalities on the EEG. We will also have real-time long-term recordings to trigger acute interventions automatically, should a seizure be detected.


Brain imaging is another mainstay in the approach to patients with epilepsy. Brain imaging techniques provide the ability to non-invasively map the structure and function of the brain. It has advanced much over the past 4 decades.
In the 1970s, x-ray CT scan was invented and gave us the first images from inside the skull.
By the late 1980s, MRI technology enabled detailed living brain visualisation, augmented by positron emission tomography (PET) showing brain function.
We are now entering an era in which all these different modalities of imaging will be integrated together, to give us a 3D picture of the brain architecture and its function, both normal and abnormal.
We now have computerised software for detecting subtle abnormalities that are not evident to the naked eye, such as subtle scarring in the hippocampus and subtle abnormalities of the way the brain was formed before birth.
Using what is called functional MRI, we can analyse how active different parts of the brain are during certain tasks, for example, movement, language, and memory. These results give us maps of the location of the parts of the brain that are involved in these tasks, and this is very useful if we are considering the possibility of surgical treatment, as it enables one to estimate the risks to the person, and to design the surgery to minimize these risks.




Medications for epilepsy have been around for over 100 years. Initially, these were called anticonvulsants, then antiepileptic drugs, and now antiseizure medications.
Looking to the future, I think that we will have personalised antiseizure medications and personalised precision medications.
In 1980, Carbamazepine and Valproate were the newest drugs for epilepsy, and the old-fashioned drugs were Phenytoin and Phenobarbital. We now recognise that Carbamazepine may have long-term adverse effects on bone and liver health, and Valproate may result in increased weight, resulting in an increased tendency to type 2 diabetes and high blood pressure.
We also recognise now that Valproate is associated with bad effects on a developing baby if the mother takes this drug during pregnancy. Consequently, Valproate is now the drug of last resort, rather than the drug of first choice, for females who may wish to have children in the future.
Current medications suppress the development of seizures, but do not do anything to the underlying tendency.
In the future, I think that we will have medications that prevent epilepsy from developing. I also expect that a more targeted approach will be possible.
Currently, drugs are given by mouth to the whole brain, all the time. In the future, I expect we will have sophisticated local delivery systems for giving medications to the specific part of the brain that generates seizures, and only when it is needed to prevent a seizure from occurring.
Surgical treatment of epilepsy has been around since the 1950s. In 1980, this was limited to severely affected individuals.
In contrast, today, an individual coming for surgery may only experience infrequent seizures. Epilepsy surgery is appropriate for about 3% of all of those who develop epilepsy: that is, for those for whom medication was not successful, and if one part of the brain can be identified as being the source of the epilepsy. In these individuals, surgery can be life-changing for the good, but it does carry some risks.
In the future, epilepsy surgery will employ keyhole techniques, avoiding opening the skull by using precise probes for tissue destruction with laser light, applying electrical stimulation, and delivering genetic anti-seizure treatments.

Genetic understanding of epilepsy has progressed dramatically. In 1980, we recognised that people with epilepsy often had a family history of epilepsy, and in many places, those with epilepsy were discouraged from having children.
We now know that it is rare for a single gene to cause epilepsy. More commonly, multiple subtle variations increase susceptibility. If an individual has such a tendency and has an insult to the brain, such as a head injury, that can give them a high risk of developing seizures.
Although genetics is increasingly complex, ultimately it promises clearer insights into the processes that give rise to epilepsy and potential treatments.
Stigma and prejudice have been an unwelcome accompaniment of epilepsy for centuries. Epilepsy has long been shrouded in myth and misunderstanding.
I recall in 1970s irrational statements such as “Jim cannot go on school trips or learn to swim as he is epileptic”. Such beliefs were often rooted in a lack of understanding and fear of the condition.
There is still a way to go, but the situation now is greatly improved with realistic risk assessments and an increased level of awareness about the condition. For example, it would not be so unusual now to have individuals with epilepsy working in medicine, nursing, or in the police force.
While epilepsy is a neurological condition, rather than a disability, it has been a protected characteristic since 2010.
There is, however, still some covert discrimination and individuals may well choose to take fewer risks, for example, by not going for a new job, just in case something goes wrong in the future.
Epilepsy diagnosis and treatment is a whole lot better than it was 40 years ago, but there is a need for further improvement and to ensure equality of access to all parts of the country and all segments of society. Precision epilepsy care and therapy are expensive, and it is very important that those treating individuals with epilepsy maintain humanity and continuity of personal interaction and support.
Charities such as The Meath Epilepsy Charity do wonderful work in ensuring that care provided to all is as good as possible, and with lobbying for improvements. Importantly for the individuals they support, The Meath is proud to recognise ability. Doing so requires an informed and measured approach to assessing risk- for example, with the correct level of support in place, residents enjoy activities such as swimming, day trips, horse riding and football.
National Epilepsy Awareness Week is an important opportunity for all UK epilepsy charities to work together to increase awareness of epilepsy. In doing so, I hope that more people will understand some of the challenges for people living with the condition, but also to further reduce stigma and prejudice. On a practical level, it is also a good opportunity to share information about what to do if someone has a seizure.
As a Patron of The Meath, it is my pleasure to have shared these insights into my 40 years of experience in neurology.
Image credit: Thank you to UCL for MRI and brain imaging pictures.
For information about what to do if someone has a Tonic- clonic seizure visit https://meath.org.uk/about-us/about-epilepsy-us/
To find out more about Professor John Duncan, visit


